Bless you all for sharing your thoughts and ideas about me, and the alternative doctor mission! I received a landslide of wonderful messages over the last week: heart-breaking, inspiring, deeply sincere, soul-warming and—in some cases—quite poetical!
I’d love to share some, but that would mean picking and choosing, which could result in a degree of judgmentalism, so maybe not.
But let me say this: the OVERWHELMING message (95%+) I received was KEEP DOING WHAT YOU ARE DOING, IT’S FINE! and WE LOVE YOU! and THANK YOU FOR ALL YOUR KNOWLEDGE.
There were some good suggestions for change too and we are taking those on board. For me—I’m just glad I am hitting the nail on the head and will keep doing what I am doing, to the best of my ability.
So, down to business for this week…
AND IT’S HORRIFIC!
I don’t just want to upset or scare you. But if you haven’t given up ALL HOPE of hospital care in your later years, it’s time you did! Just forget it, I would!
The truth is, hospitals just cannot cope with what they are asked to do. It’s not the doctors or nurses. It’s miserable below-par staffing levels, brought about by the suits (the controlling accountants), trying to increase profits to the max, while letting patient care go hang.
I don’t know how it is in Britain these days—I’ve heard alarming reports that the beloved National Health Service (NHS) has all but collapsed under the strain (meanwhile, the suits keep paying themselves bigger and bigger salaries).
But in the USA it’s reached such a pitch… it’s called “boarding”, meaning patients left without a bed, parked on gurneys, trolleys and wheelchairs, dumped in side rooms, corridors or on the floor for hours, days… even WEEKS! It’s unbelievable.
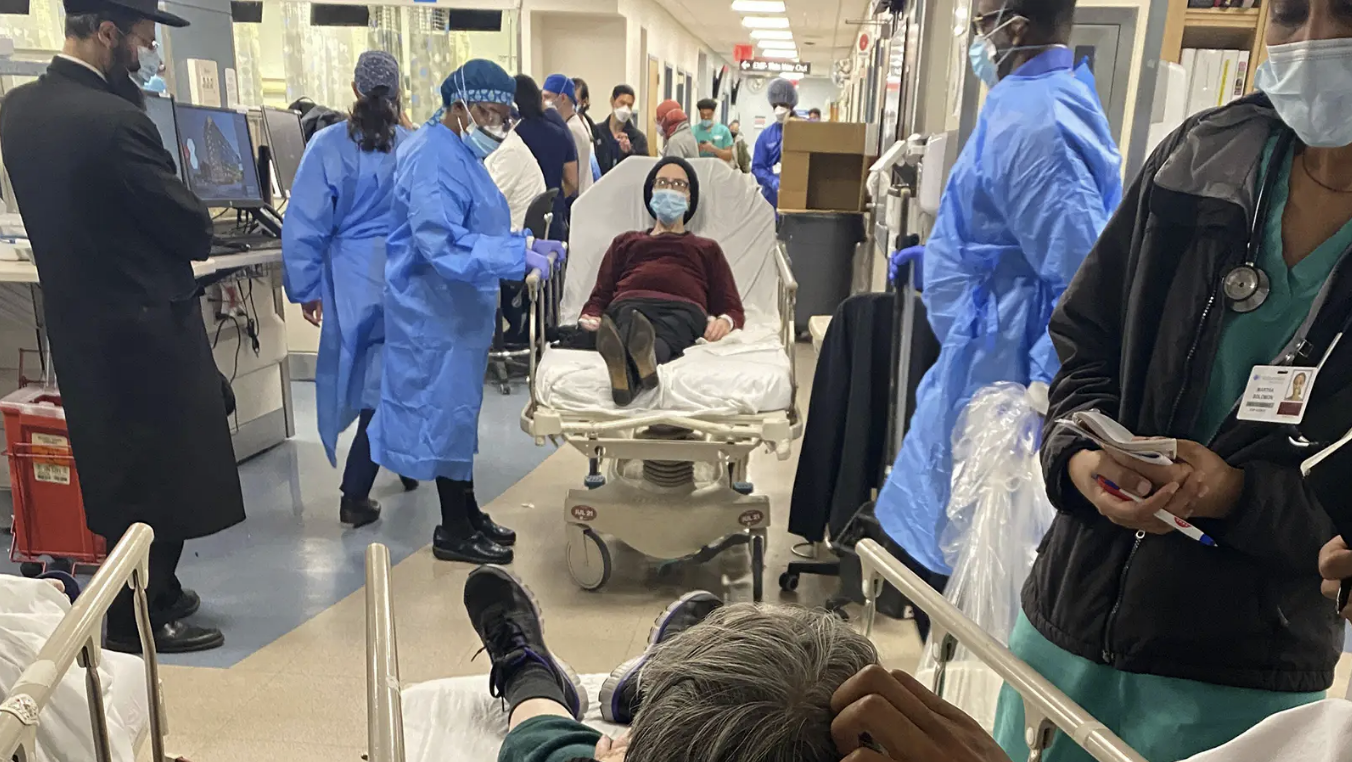
A recent survey by the American College of Emergency Physicians (ACEP) invited ER doctors to share what they’ve seen happen as a result of ER boarding. Patients with brain bleeds, hip fractures, and even necrotizing genital infections were being treated publicly in the waiting room because there were no rooms or even hallway beds available in the ER.
Multiple physicians shared stories of patients dying in the waiting room because the ER was so overwhelmed, they had to wait for hours to see a physician. One survey showed 10% of patients went home, without actually being attended to at all!
A recent commentary in the New England Journal of Medicine identified “misaligned healthcare economics” as one of the primary drivers of boarding. Sounds like some sort of explanation. But is it?
Not really. We call it greed. It is better business for hospitals to keep their beds available for surgical patients who bring in more money, instead of leaving some spare capacity for likely surges of ER patients. If more than 90% of beds are full upstairs on Sunday, hospital revenues may be optimized, but a dangerous ER gridlock becomes inevitable.
It Should Not Be
A special session of Congress was called 35 years ago to make lawmakers and the public aware of stories of patients left to die in hospital parking lots for lack of insurance. They couldn’t pay and so were left to die WITHOUT BEING ADMITTED.
Around the time of that congressional testimony, called “Equal Access to Health Care: Patient Dumping,” a new guarantee came about: that any individual who comes to the emergency room (ER) must be given a medical screening evaluation and appropriate stabilization. This enshrines ER availability in federal law, as a right.
So the patient MUST be admitted. But what happens if hospital management don’t make beds available? Where are the patients’ rights? This is what is called “boarding,” and it is an ever-present threat to the role in the resuscitative care of the sickest patients. As the mismatch between acute care needs and available capacity mounts, the staff work load descends to chaos.
There is supposed to be a recommended 4-hour maximum boarding time (but we’re way past that on a good day, said one desperate doctor). The trouble is there is no accountability and no mandatory reporting requirements.
The problem isn’t just physical space—it’s staff. Nurses, crushed under the weight of a profit-driven staffing crisis, must now care for both admitted boarding patients and the steady stream of new patients. In practice, there are often no limits on staffing ratios for ER nurses. On the medical floor, a single nurse may have four to five patients. In the ICU, two patients. In the ER, a single nurse is often asked to cover 10 or more patients. Some critically ill cases are “admitted” but in the ER waiting for an ICU bed, without regard for the safety or sustainability of this arrangement.
My friend Graham Simpson MD and his buddy Graham Wilson MD—both from the same university in South Africa—started the first and best ER in Southern Nevada, right here in Las Vegas. Here’s what he has to say about the current situation.
 Graham Simpson
Graham Simpson
In those days we worked pretty hard. Sometimes the pressure and stress was immense. But we got through. Patients never had to wait for more than a few hours for a bed. The picture today is so dismal, I’m just appalled. How can today’s doctors live with this?
What is HHS doing? Not a lot, it seems. There is too much emphasis on money and too many doctors thinking their role is making money for shareholders, rather than relieve suffering.
All this makes me personally very sad, because some of the happiest days of my hospital years were working in ER or “Casualty” as the Brits called it then. I would see over 100 patients a shift sometimes—and a “shift” could sometimes be as long as 6.00 pm on Friday to 8.00 am Monday morning! Quick-witted decision-making was essential. It was great to save lives and I suppose I lost plenty. You can’t win them all as the saying goes.
But I don’t recall that it ever took more than a few hours to get patients needing admission up onto the “wards” (floors).
Come to think of it, those were some of the last times I wore a white coat, as opposed to a suit and tie! Haha!
To your good health,
Prof. Keith Scott-Mumby
The Official Alternative Doctor
[based on a piece in MedPageToday by Alexander T. Janke, MD, MHS, Jennifer Tsai, MD, Med, and Kristen Panthagani, MD, PhD February 19, 2023]
The post Thank You From The Heart! appeared first on Dr. Keith Scott-Mumby.
